Vocal cord nodules, commonly referred to as “singer’s nodes” or “teacher’s nodes,” are benign, callus-like growths that develop on the vocal cords due to repetitive trauma or misuse. These non-cancerous lesions typically appear symmetrically on both vocal cords and can significantly impair voice quality if not managed properly. Fortunately, with early intervention and appropriate treatment, most cases resolve completely without permanent damage.
What Are Vocal Cord Nodules? — Definition & Overview
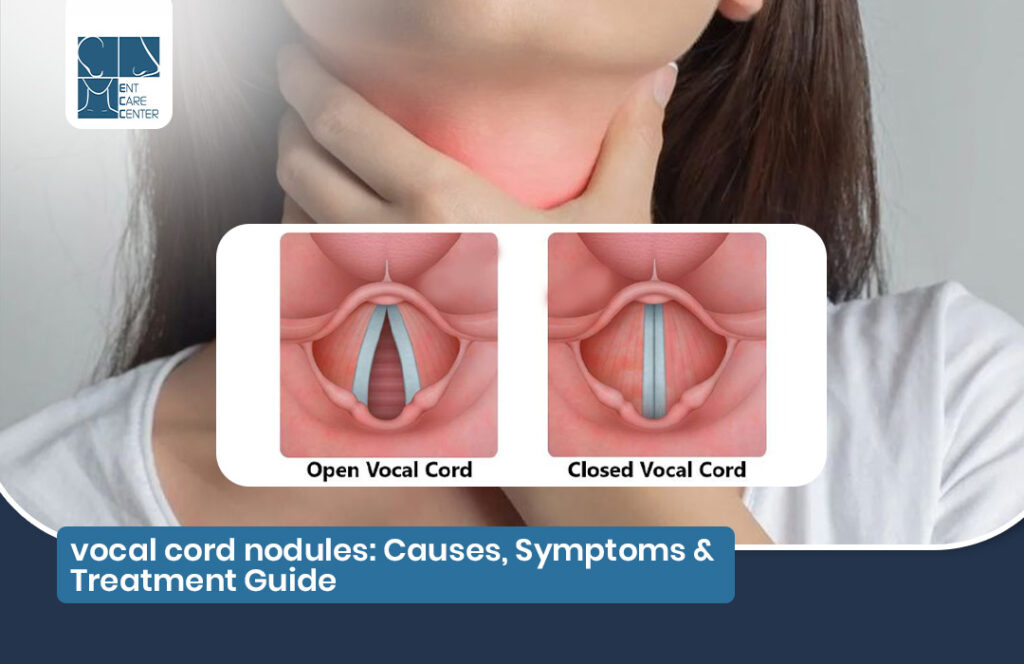
Vocal cord nodules are small, thickened areas of tissue that form on the edges of the vocal folds (commonly called vocal cords) at the point where they collide most forcefully during phonation. They start as soft, swollen areas from acute inflammation but gradually become firmer and more fibrous with continued abuse, resembling calluses on the skin.
Unlike vocal cord polyps (which are usually unilateral, fluid-filled, and more fragile) or cysts (encapsulated fluid collections), nodules are almost always bilateral and symmetric. They interfere with the precise closure and vibration of the vocal cords, leading to irregular airflow and turbulent sound production. While benign and never cancerous in typical cases, untreated nodules can lead to scarring or chronic dysphonia (voice disorders).
Primary Causes of Vocal Cord Nodules
The fundamental cause is chronic vocal fold trauma from forceful or prolonged vibration. Key triggers include:
- Excessive loud speaking, yelling, or singing for extended periods
- Speaking or singing in an inappropriate pitch (too high or too low for the individual’s natural range)
- Habitual forceful throat clearing, coughing, or grunting
- Prolonged talking in noisy environments without amplification
- Intense vocal demands without adequate warm-up or rest
Secondary irritants that exacerbate tissue vulnerability include:
- Gastroesophageal reflux disease (GERD) or laryngopharyngeal reflux (LPR), where stomach acid reaches the throat
- Smoking or exposure to secondhand smoke
- Chronic allergies or post-nasal drip causing inflammation
- Dehydration or dry air environments
- Endocrine factors, such as hypothyroidism, which can alter vocal fold tissue
Risk Factors & Who Is Most Likely to Get Them
Certain populations and behaviors significantly increase susceptibility:
- Occupational voice users: Teachers (especially elementary), singers, coaches, clergy, telemarketers, salespeople, and aerobic instructors
- Children: Particularly energetic boys aged 5–10 who frequently shout during play
- Women aged 20–50: Slightly higher incidence, possibly due to smaller larynx size and higher fundamental speaking frequency
- Individuals with untreated reflux, allergies, or sinus issues
- Smokers and those with chronic respiratory conditions
- People under chronic stress, leading to increased muscle tension and strained phonation
Common Symptoms of Vocal Cord Nodules
Symptoms typically develop gradually and worsen with continued voice use:
- Persistent hoarseness or roughness in the voice
- Breathy or airy voice quality with air escape
- Reduced vocal endurance — voice fatigues quickly after minimal use
- Loss of upper vocal range (difficulty hitting high notes)
- Pitch breaks or sudden voice cut-outs
- Sensation of a lump, tightness, or pain in the throat during speaking
- Increased effort required to produce voice
- Frequent throat clearing or coughing to “reset” the voice
Symptoms lasting more than 2–3 weeks, especially in high-risk individuals, warrant professional evaluation to rule out more serious conditions.
How Vocal Cord Nodules Are Diagnosed
Accurate diagnosis requires specialized examination:
- Comprehensive voice history assessing occupational demands, habits, and associated conditions
- Head and neck examination
- Flexible or rigid laryngoscopy: Allows direct visualization of the vocal cords
- Videostroboscopy: Gold standard — uses strobe light to capture slow-motion vibration patterns, revealing the characteristic “hourglass” closure defect caused by nodules
- Acoustic and aerodynamic voice analysis to quantify severity
- Rarely, biopsy if appearance is atypical (to exclude dysplasia or malignancy)
Early diagnosis is crucial, as small, soft nodules respond far better to conservative treatment than mature, fibrotic ones.
Non-Surgical Treatment Options
The cornerstone of treatment is behavioral and medical management, with surgery reserved as a last resort:
- Absolute or relative voice rest: Brief periods of minimal talking to reduce inflammation
- Voice therapy with a qualified speech-language pathologist (SLP): Focuses on eliminating abusive behaviors, improving vocal efficiency, and teaching resonant voice techniques (e.g., resonant voice therapy, vocal function exercises)
- Management of contributing medical conditions:
- Aggressive reflux control (diet modification, PPIs, elevated head sleeping)
- Allergy treatment and nasal hygiene
- Smoking cessation
- Optimal hydration (8–10 glasses of water daily) and environmental humidification
- Vocal pacing strategies for professional voice users
With consistent therapy (typically 6–12 sessions), 80–90% of patients experience significant improvement or complete resolution within months.
When Surgery Is Considered
Surgical intervention (micro-laryngoscopy with phonomicrosurgery) is rarely indicated for nodules and only considered when:
- Nodules are large, mature, and fibrotic
- Symptoms persist despite 3–6 months of optimal voice therapy and medical management
- Professional voice demands cannot be met with conservative measures
The procedure involves precise cold-instrument or laser removal under general anesthesia. Post-operative voice therapy is mandatory to prevent recurrence and optimize healing. Outcomes are generally excellent when combined with behavioral change.
Prevention Tips & Vocal Health Best Practices
Prevention centers on vocal hygiene and smart voice use:
- Drink adequate water throughout the day; avoid excessive caffeine and alcohol
- Use amplification (microphones) in noisy settings or large groups
- Avoid habitual yelling, screaming, or whispering
- Warm up the voice before prolonged or demanding use
- Practice good posture and relaxed breathing to reduce laryngeal tension
- Treat reflux, allergies, and respiratory issues promptly
- Quit smoking and minimize exposure to irritants
- Take regular voice breaks during heavy use periods
- Learn and maintain healthy vocal technique through periodic coaching
Daily Life & Management Strategies
For those with nodules or at risk:
- Monitor voice quality daily and rest at first signs of fatigue
- Use non-vocal signals (whistles, bells, gestures) when possible
- Replace throat clearing with silent swallow or gentle hum
- Employ resonant voice techniques in conversation (forward-focused, easy onset)
- Schedule regular follow-ups with ENT and SLP if in a high-risk profession
- Incorporate neck, shoulder, and jaw relaxation exercises
Long-term adherence to these habits dramatically reduces recurrence risk.
Prognosis: What to Expect & Long-Term Outlook
The prognosis for vocal cord nodules is highly favorable:
- With early intervention and compliance, most patients regain normal or near-normal voice function
- Complete resolution is common for soft, recent nodules
- Even chronic cases show marked improvement with dedicated therapy
- Recurrence risk is low when abusive behaviors are permanently modified
- Rare complications (permanent scarring or persistent dysphonia) usually result from delayed treatment or non-compliance
Professional voice users can typically return to full performance capacity with proper management. Early consultation with an otolaryngologist and voice-specialized speech therapist offers the best chance for complete recovery and long-term vocal health.
If you experience persistent voice changes, seek evaluation promptly — protecting your voice today ensures its strength tomorrow.